What is plasma and what are platelets?
Plasma is the liquid portion of whole blood. It is composed largely of water and proteins, and it provides a medium for red blood cells, white blood cells and platelets to circulate through the body. Platelets, also called thrombocytes, are blood cells that cause blood clots and other necessary growth healing functions.
Platelet activation plays a key role in the body’s natural healing process.
What is platelet-rich plasma (PRP) and what are PRP injections?
Platelet-rich plasma (PRP) is a growth factor rich medium that is developed from the patient’s blood. It is not synthetic. PRP therapy uses injections of a concentration of a patient’s own platelets to accelerate the healing of injured tendons, ligaments, muscles and joints. In this way, PRP injections use each individual patient’s own healing system to improve musculoskeletal problems.
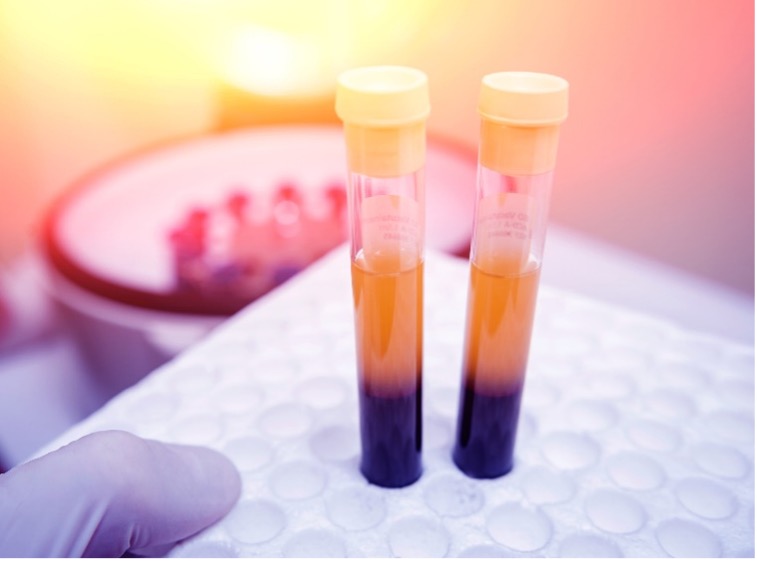
PRP injections are prepared by taking anywhere from one to a few tubes of your own blood and running it through a centrifuge to concentrate the platelets. These activated platelets are then injected directly into your injured or diseased body tissue. This releases growth factors that stimulate and increase the number of reparative cells your body produces.
Research has shown PRP to be effective in the management of early osteoarthritis (joint degeneration) and some tendon injuries.
How are PRP injections done? What is involved?
PRP therapy involves one (for tendons) or two injections (for joints) into the injured area a fortnight apart. On each occasion the patient will be required to donate blood for generation of the PRP. Injections are done under sterile conditions, with local anaesthetic and using ultrasound guidance. Each procedure will take approximately 30 minutes.
We published a research paper in 2022 showing that two injections of PRP for knee osteoarthritis reduces symptoms in the majority of cases. We also showed that three injections (or more) were not more effective than two.
What do I need to do before my injections?
Patients are required to cease taking anti-inflammatory tablets one week prior to the PRP procedure. Patients taking regular aspirin should continue to take this.
What do I need to do after my injections?
It is recommended that someone drive the patient home after an injection due to some potential residual effects of the local anaesthetic or discomfort from the procedure. Depending on the structure injected, the patient may need to offload the area for a period.
Patients undergoing PRP injections should also be actively involved in a supervised rehabilitation program. In some instances, the patient may need to stop exercise for a period and resume after medical review.
Risks
In general, adverse outcomes from PRP injections are rare, but they may include:
Bleeding/Bruising/Infection
To reduce chance of infection all injections are done under sterile conditions using ultrasound guidance for accuracy. PRP has natural anti-bacterial properties that reduce chance of infection.
Pain/Discomfort
Injections can be uncomfortable. In all cases, local anaesthetic is used. Patients are encouraged to use simple analgesia (Panadol/Panadeine) as required after the procedure and icing can be very helpful. If necessary, the doctor can provide a prescription for Panadeine Forte. Much of the post procedure discomfort can be addressed by closely following any post procedure instructions.
Contra-Indications
PRP injections are generally very safe, but are contra-indicated in the following conditions:
- Pregnancy
- Cancer
- Some bleeding disorders
More information/evidence for PRP?
The use of intra‐articular platelet rich plasma for the symptomatic management of osteoarthritis of the knee: a pilot study. Sibillin O, Mitchell D, Harris G et al. ANZ J Surg (2022) doi:10.1111/ans.17565




